Powder coating for medical devices and healthcare equipment occupies a unique position in the coatings industry — one where coating performance directly affects patient safety, infection control, and regulatory compliance. The coating on a hospital bed rail, surgical instrument tray, or diagnostic equipment housing must not only protect the metal substrate from corrosion and wear but must also be biocompatible (non-toxic to human tissue), resistant to repeated sterilization cycles, compatible with aggressive hospital cleaning chemicals, and manufactured under quality management systems that meet the rigorous requirements of medical device regulations.
Technical
Powder Coating Medical Devices and Equipment: Biocompatibility, Sterilization Resistance, and Regulatory Compliance
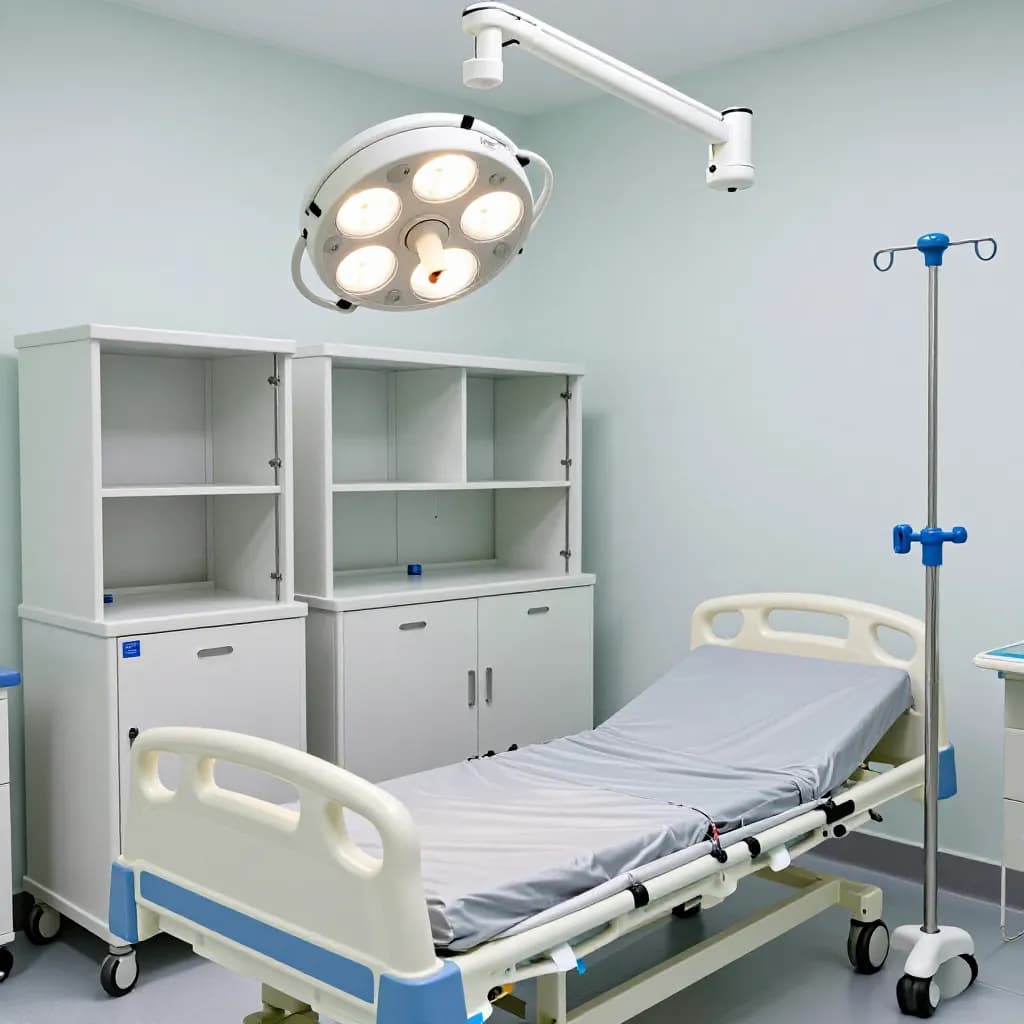
The medical device coating market spans a wide range of applications, from Class I devices (low risk — hospital furniture, examination tables, IV poles) through Class II devices (moderate risk — powered surgical instruments, diagnostic equipment housings, patient monitoring enclosures) to selected Class III devices (high risk — implant delivery systems, surgical robot components). Each device classification carries different regulatory requirements for the coating, with higher-risk devices requiring more extensive biocompatibility testing and quality documentation.
Ready to Start Your Project?
From one-off customs to 15,000-part production runs — get precise pricing in 24 hours.
On This Page
Medical Device Coating: Where Performance Meets Patient Safety
Powder coating's advantages for medical applications include its dense, non-porous film structure that resists bacterial colonization, its chemical inertness after full cure that minimizes extractable and leachable substances, and its manufacturing process that eliminates solvent residues that could compromise biocompatibility. These inherent properties, combined with the ability to formulate powder coatings with specific antimicrobial, chemical resistance, and sterilization resistance properties, have made powder coating the preferred finish for a growing range of medical devices and healthcare equipment.
Biocompatibility Testing and ISO 10993 Compliance
Biocompatibility — the ability of a material to perform with an appropriate host response in a specific application — is the foundational requirement for any coating used on medical devices. ISO 10993 (Biological Evaluation of Medical Devices) provides the framework for biocompatibility assessment, defining a series of tests that evaluate the coating's potential to cause cytotoxicity (cell death), sensitization (allergic reaction), irritation, systemic toxicity, genotoxicity, and other adverse biological responses.
The specific biocompatibility tests required for a powder-coated medical device depend on the nature and duration of body contact, as defined in ISO 10993-1. Surface-contacting devices with limited contact duration (less than 24 hours) — such as hospital bed rails, examination table surfaces, and equipment housings — typically require cytotoxicity testing (ISO 10993-5), sensitization testing (ISO 10993-10), and irritation testing (ISO 10993-23). Devices with prolonged or permanent body contact require additional testing including systemic toxicity, genotoxicity, and implantation studies.
Cytotoxicity testing per ISO 10993-5 is the most fundamental biocompatibility test and is required for virtually all medical device coatings. The test evaluates whether extractable substances from the coating cause death or damage to cultured mammalian cells. Fully cured TGIC-free polyester and epoxy powder coatings consistently pass cytotoxicity testing because the thermoset cross-linking reaction consumes reactive components, leaving a chemically inert film with minimal extractable content.
It is important to note that biocompatibility is a property of the complete coating system — not just the powder formulation. The pretreatment chemicals, cure conditions, and any post-coating treatments all affect the biocompatibility of the finished device. A powder coating that passes biocompatibility testing when applied over one pretreatment system may not pass when applied over a different pretreatment. Medical device manufacturers must validate biocompatibility for their specific coating process, not rely solely on powder manufacturer data.
Sterilization Resistance: Autoclave, Gamma, and Chemical Methods
Medical devices and equipment must be sterilized to prevent healthcare-associated infections, and the coating must withstand repeated sterilization cycles without degradation, discoloration, adhesion loss, or release of extractable substances. The three primary sterilization methods — steam autoclave, gamma irradiation, and chemical sterilization — each impose different stresses on the coating that must be addressed through appropriate formulation and testing.
Steam autoclave sterilization (121°C at 15 psi for 15-30 minutes, or 134°C at 30 psi for 3-4 minutes) is the most common sterilization method for reusable medical devices and equipment. The combination of high temperature, high pressure, and saturated steam creates an extremely aggressive environment for organic coatings. Standard polyester powder coatings can withstand occasional autoclave exposure, but repeated cycling (100+ cycles) can cause hydrolytic degradation of the polyester resin, leading to gloss loss, chalking, and eventually adhesion failure. Autoclave-resistant powder coatings use modified polyester or epoxy-polyester hybrid resins with enhanced hydrolysis resistance, typically validated for 500+ autoclave cycles at 134°C without significant degradation.
Gamma irradiation sterilization (typically 25-50 kGy dose) is used for single-use medical devices and some reusable equipment. Gamma radiation causes chain scission and cross-linking in polymer coatings, which can lead to embrittlement, discoloration (yellowing), and changes in mechanical properties. Epoxy powder coatings are more resistant to gamma irradiation than polyester formulations, maintaining their mechanical properties and appearance at doses up to 50 kGy. For devices requiring gamma sterilization, the coating should be validated at the maximum expected cumulative radiation dose.
Chemical sterilization using ethylene oxide (EtO), hydrogen peroxide plasma (Sterrad), or peracetic acid is used for heat-sensitive devices. These methods are generally less aggressive to powder coatings than autoclave or gamma sterilization, but the coating must be tested for compatibility with the specific sterilant. Hydrogen peroxide plasma, in particular, can cause surface oxidation and discoloration of some powder coating formulations. Chemical resistance testing per ASTM D1308 with the specific sterilant at use concentration and exposure time validates coating compatibility.
Hospital Beds, Stretchers, and Patient Care Furniture
Hospital beds, stretchers, examination tables, and patient care furniture represent the largest volume category of medical powder coating. These devices are fabricated from steel tube and sheet metal and must withstand the demanding hospital environment — frequent cleaning with aggressive disinfectants, impact from bed rails and equipment carts, body fluid exposure, and the mechanical stress of patient handling and bed adjustment mechanisms.
The coating specification for hospital beds typically requires polyester or epoxy-polyester hybrid powder at 60-100 microns over zinc phosphate pretreatment. The coating must pass chemical resistance testing with hospital-grade disinfectants including quaternary ammonium compounds, sodium hypochlorite (bleach) at 1:10 dilution, hydrogen peroxide at 3%, and accelerated hydrogen peroxide formulations. These disinfectants are used multiple times daily on patient care surfaces, and the coating must maintain its appearance and adhesion through thousands of cleaning cycles over the bed's 10-15 year service life.
Color selection for hospital furniture is driven by both functional and psychological considerations. White and light grey remain the most common colors for clinical environments, providing a clean appearance and facilitating visual inspection for contamination. However, healthcare design research has demonstrated that color can positively affect patient outcomes — calming blues and greens in patient rooms, warm neutrals in rehabilitation areas, and bright accents in pediatric wards. Powder coating's extensive color range enables healthcare furniture manufacturers to offer the full spectrum of evidence-based healthcare color palettes.
Antimicrobial powder coatings with silver ion technology are increasingly specified for hospital bed rails, side tables, and other high-touch surfaces. These coatings provide continuous antimicrobial activity that supplements manual cleaning, reducing the microbial burden on surfaces between cleaning cycles. Clinical studies have demonstrated that antimicrobial copper and silver surfaces can reduce healthcare-associated infection rates, though the contribution of coated surfaces versus other infection control measures is still being quantified.
Surgical Instruments, Trays, and Sterilization Containers
Surgical instrument trays, sterilization containers, instrument organizers, and selected surgical instruments are powder coated for identification, corrosion protection, and ergonomic purposes. These components face the most demanding sterilization requirements in the medical coating spectrum — hundreds to thousands of autoclave cycles at 134°C over their service life, combined with exposure to enzymatic cleaners, ultrasonic cleaning solutions, and mechanical washing in automated reprocessing equipment.
Color coding of surgical instrument trays and containers is a critical safety application of powder coating in the operating room. Different colors identify instrument sets for specific surgical procedures, departments, or sterilization status, reducing the risk of wrong-instrument errors and improving workflow efficiency. The color coding system must be maintained through hundreds of sterilization cycles, requiring powder coatings with exceptional autoclave resistance and color stability at elevated temperatures.
The coating on surgical instrument handles serves an ergonomic function — providing a non-slip grip surface that maintains tactile feedback while wearing surgical gloves. Textured powder coatings with controlled surface roughness (Ra 5-15 micrometers) provide effective grip enhancement without creating surface features that could harbor bacteria or impede cleaning. The texture must be fine enough to be thoroughly cleaned in automated reprocessing equipment while coarse enough to provide meaningful grip improvement.
Sterilization container coating must withstand not only the thermal and chemical stresses of autoclave processing but also the mechanical stresses of stacking, transport, and handling in the central sterile supply department. Impact resistance of 80+ inch-pounds (direct and reverse) and pencil hardness of 2H or greater are typical requirements. The coating must also be compatible with the silicone gaskets used to seal sterilization containers, without causing gasket degradation or adhesion that could compromise the container's sterile barrier function.
Diagnostic Equipment and Laboratory Instrument Housings
Diagnostic imaging equipment (MRI, CT, X-ray), laboratory analyzers, patient monitors, and other electronic medical devices require powder-coated housings that provide environmental protection for sensitive electronics while meeting the aesthetic, safety, and regulatory requirements of the healthcare environment. These housings must be visually consistent, easy to clean, resistant to chemical exposure, and compliant with electromagnetic compatibility (EMC) requirements.
MRI (magnetic resonance imaging) environments present a unique coating challenge. The powerful magnetic field of an MRI scanner (1.5-7 Tesla) attracts ferromagnetic materials with potentially lethal force. All equipment and furniture in the MRI suite must be non-ferromagnetic, typically fabricated from aluminum, stainless steel (non-magnetic grades 304 and 316), or non-metallic materials. The powder coating on MRI-compatible equipment must also be free of ferromagnetic pigments — iron oxide pigments commonly used in red, brown, and black powder coatings are ferromagnetic and must be replaced with non-magnetic alternatives (carbon black for black, organic pigments for colors) in MRI-safe formulations.
Laboratory instrument housings face chemical exposure from reagents, solvents, and biological specimens that can be more aggressive than standard hospital cleaning chemicals. Concentrated acids, bases, organic solvents (acetone, methanol, xylene), and biological staining agents (Giemsa, Wright's, Gram stain) can attack standard polyester powder coatings. Epoxy or epoxy-polyester hybrid powder coatings provide superior chemical resistance for laboratory applications, though they must be protected from UV exposure if the equipment is located near windows.
Electrostatic discharge (ESD) protection is required for housings that enclose sensitive electronic components. Standard powder coatings are electrical insulators with surface resistivity above 10^12 ohms per square, which can accumulate static charges that discharge into enclosed electronics. ESD-dissipative powder coatings with surface resistivity in the range of 10^6 to 10^9 ohms per square safely dissipate static charges without the risk of spark discharge. These formulations are specified for electronic medical device housings where ESD could affect device performance or patient safety.
FDA Regulation and ISO 13485 Quality Management
Medical device coatings in the United States are regulated by the FDA under 21 CFR (Code of Federal Regulations), with specific requirements depending on the device classification and intended use. The coating is considered a component of the medical device and must be included in the device's design history file, risk analysis, and quality management system documentation. For devices that contact patients, the coating must be evaluated for biocompatibility per FDA guidance on ISO 10993.
ISO 13485 (Medical Devices — Quality Management Systems) is the international quality management standard for medical device manufacturing, and its requirements extend to coating suppliers and subcontractors. Powder coating facilities serving the medical device industry must either hold ISO 13485 certification themselves or operate under the quality management system of their medical device manufacturer customer. Key ISO 13485 requirements for coating operations include documented procedures for all coating processes, validated process parameters (pretreatment chemistry, cure temperature and time, film thickness), traceability of coating materials to specific device lots, and controlled handling of nonconforming product.
Process validation is a fundamental requirement for medical device coating operations. Unlike standard industrial coating where quality is verified by testing the finished product, medical device regulations require that the coating process itself be validated to consistently produce acceptable results. This involves Installation Qualification (IQ — verifying equipment is properly installed), Operational Qualification (OQ — verifying the process operates within specified parameters), and Performance Qualification (PQ — verifying the process consistently produces product meeting all specifications). Process validation must be repeated whenever significant changes are made to equipment, materials, or process parameters.
Design controls per 21 CFR 820.30 require that the coating specification be established through a systematic design process that includes design input (performance requirements), design output (coating specification), design verification (testing that the coating meets the specification), and design validation (confirmation that the coated device meets user needs). This design control documentation becomes part of the device's design history file and must be maintained for the life of the device.
Infection Control Coatings and Emerging Healthcare Technologies
The healthcare industry's focus on infection prevention is driving innovation in antimicrobial and easy-clean powder coating technologies for medical devices and healthcare environments. Beyond the silver ion antimicrobial coatings discussed earlier, several emerging coating technologies are being developed and validated for healthcare applications.
Copper-infused powder coatings leverage the inherent antimicrobial properties of copper, which has been registered by the EPA as the first solid antimicrobial material. Copper surfaces continuously kill bacteria through a mechanism involving copper ion release and reactive oxygen species generation. Powder coatings incorporating copper particles or copper alloy pigments can provide similar antimicrobial activity, with the advantage of color flexibility and corrosion protection that bare copper surfaces lack. Clinical trials of copper-containing surfaces in hospital settings have demonstrated significant reductions in surface microbial burden and healthcare-associated infection rates.
Photocatalytic powder coatings incorporating titanium dioxide (TiO2) nanoparticles provide antimicrobial and self-cleaning properties activated by UV or visible light. When illuminated, the TiO2 photocatalyst generates reactive oxygen species that decompose organic contaminants and kill microorganisms on the coating surface. These coatings are particularly promising for healthcare environments with adequate lighting, providing continuous surface decontamination without chemical agents.
Hydrophobic and superhydrophobic powder coatings with water contact angles above 150° are being developed for medical applications where fluid repellency is beneficial — surgical instrument surfaces that resist blood adhesion, equipment housings that shed cleaning solutions, and surfaces that resist biofilm formation. These coatings use fluoropolymer chemistry or nano-structured surface textures to achieve extreme water repellency, though their long-term durability under the mechanical and chemical stresses of healthcare environments is still being validated.
The convergence of coating technology with digital health is also creating new requirements. Smart hospital beds with integrated sensors, connected diagnostic equipment with IoT capabilities, and robotic surgical systems with complex electromechanical interfaces all require coatings that are compatible with embedded electronics, wireless communication systems, and sensor technologies while maintaining the biocompatibility and sterilization resistance required for medical use.
Frequently Asked Questions
What biocompatibility testing is required for powder-coated medical devices?
ISO 10993 defines the testing framework based on body contact type and duration. Surface-contacting devices typically require cytotoxicity (ISO 10993-5), sensitization (ISO 10993-10), and irritation testing (ISO 10993-23). Fully cured TGIC-free powder coatings consistently pass these tests due to their chemically inert thermoset film structure.
Can powder coating withstand autoclave sterilization?
Standard polyester powders tolerate occasional autoclaving, but repeated cycling causes hydrolytic degradation. Autoclave-resistant formulations using modified polyester or epoxy-polyester hybrid resins are validated for 500+ cycles at 134°C. These specialty powders are essential for reusable surgical instruments, trays, and sterilization containers.
What quality system is required for medical device powder coating?
ISO 13485 quality management is required, either held by the coating facility or operated under the device manufacturer's system. Requirements include documented procedures, validated processes (IQ/OQ/PQ), material traceability, and design controls per 21 CFR 820.30. Process validation must be repeated for any significant process changes.
Are antimicrobial powder coatings effective in hospitals?
Silver ion antimicrobial powder coatings demonstrate 99.9% bacterial reduction per ISO 22196 testing. Clinical studies show antimicrobial surfaces reduce microbial burden between cleaning cycles. However, they supplement rather than replace manual cleaning and disinfection. EPA FIFRA registration is required for antimicrobial claims in the US.
Can powder coating be used on MRI-compatible equipment?
Yes, but the formulation must be free of ferromagnetic pigments. Standard iron oxide pigments (used in reds, browns, and some blacks) are ferromagnetic and must be replaced with non-magnetic alternatives like carbon black or organic pigments. All MRI-suite equipment coatings should be verified for magnetic susceptibility before use.
Ready to Start Your Project?
From one-off customs to 15,000-part production runs — get precise pricing in 24 hours.